1) Adopt Best Practice Initiatives
a) Adopt UTI Best Practice
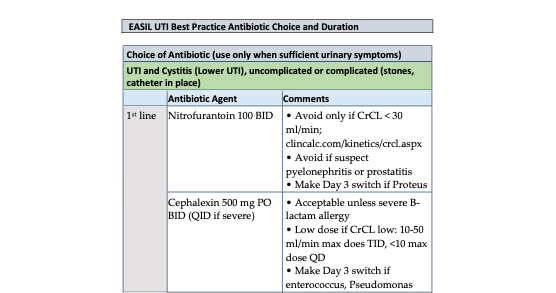
Urine testing and antimicrobial therapy should only be ordered in those with UTI symptoms, but not those with only nonspecific signs or noninfectious symptoms such as fatigue or delirium. Both unnecessary urine testing and antimicrobial therapy contribute to direct patient harm and antimicrobial resistance. Observation and monitoring of residents in whom the diagnosis of UTI is unclear is a best practice.
Download UTI Best Practice Components
for initiation of antibiotics for suspected UTI.
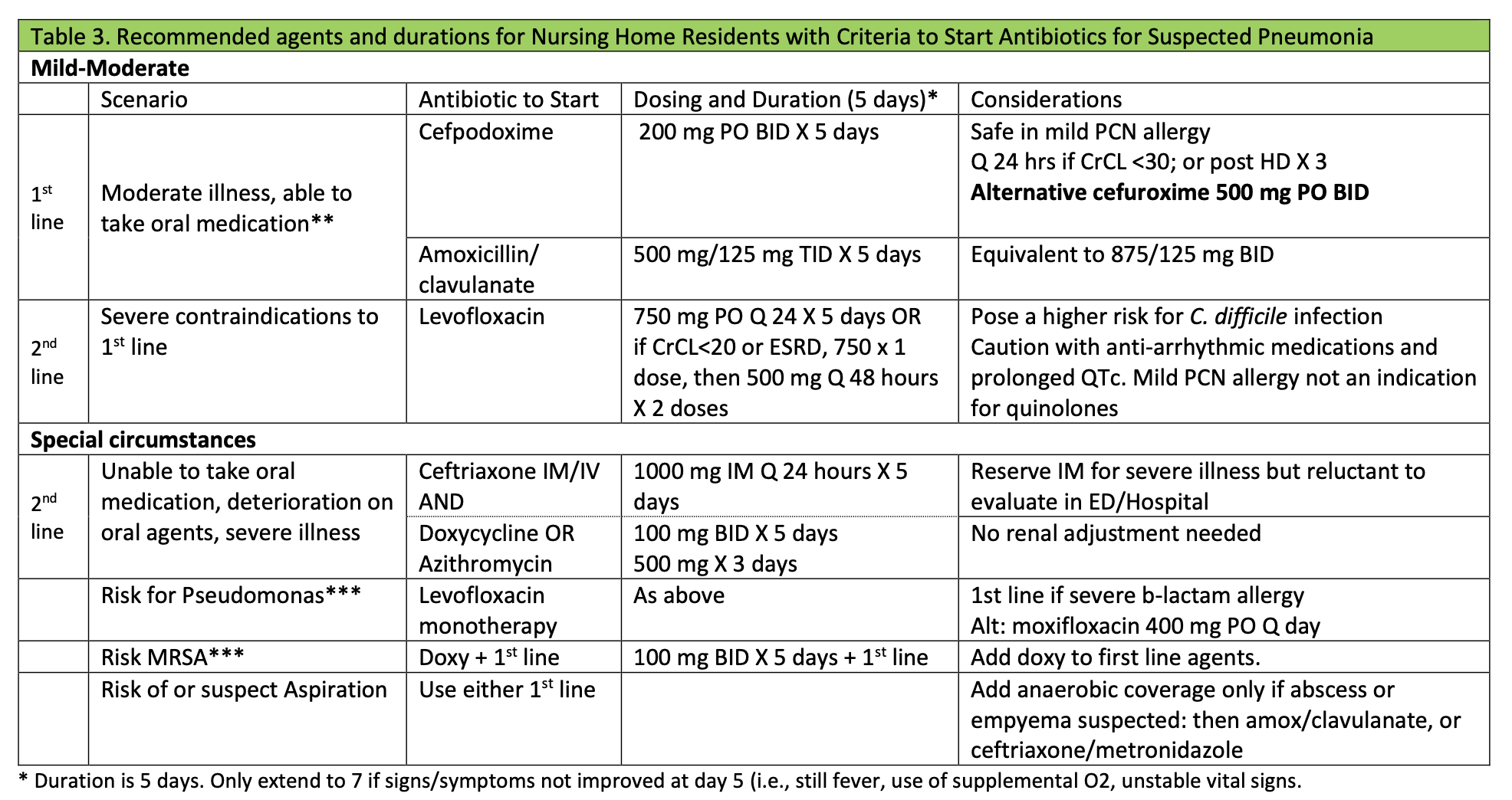
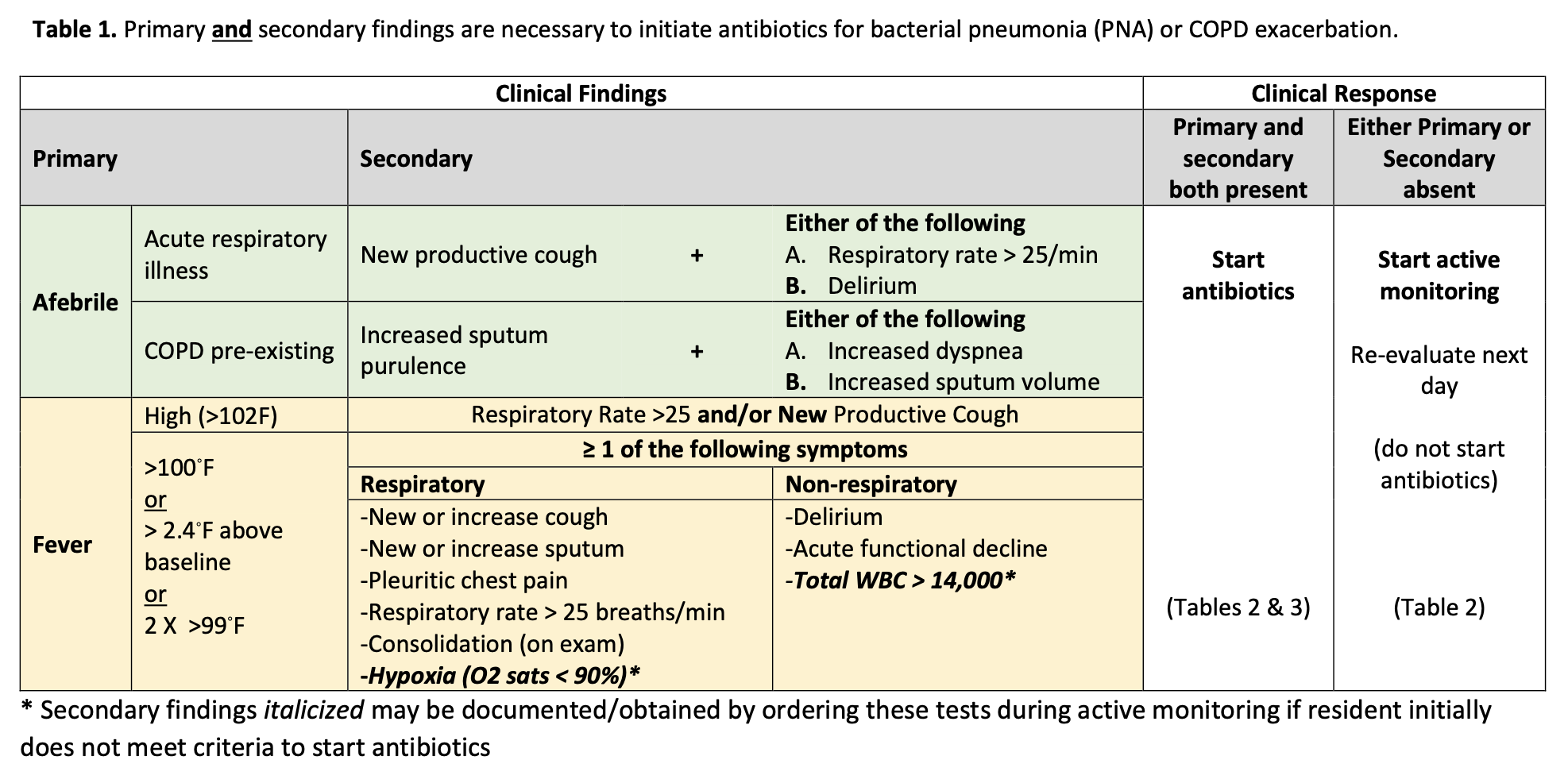
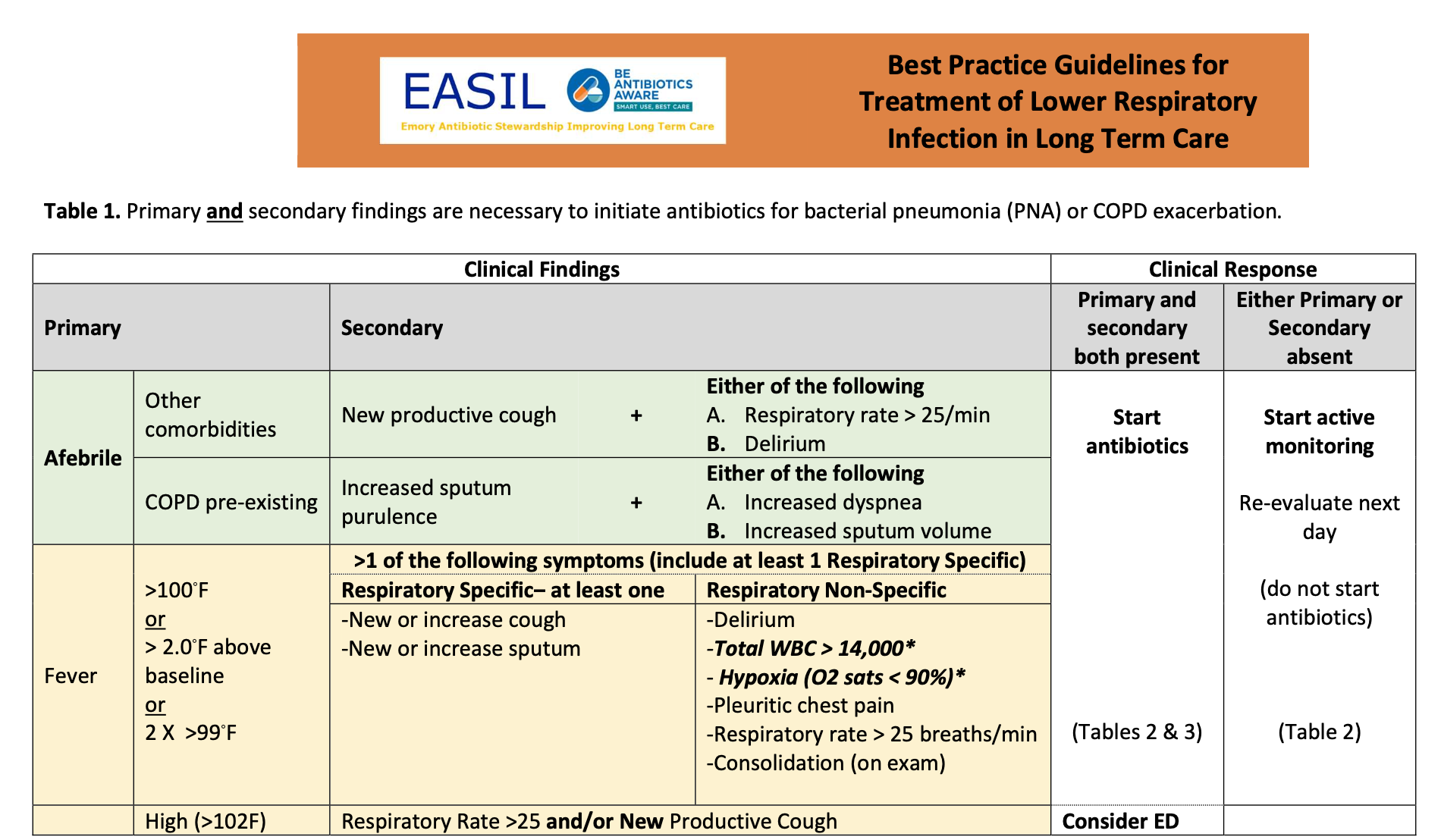
b) Adopt LRI Best Practice
The decision to treat patients with suspected LRI depends on many factors. Best practices like Active Monitoring and proper dosing have been shown to reduce overprescribing and patient harm. EASIL has developed tools to help your program implement these best practices - in the form of guidelines, pocket cards for in clinic, and an informational video.
Download LRI Best Practice Components
For easy reference during clinic, download and keep the pocket card-sized version of the LRI Best Practice guidelines.
Watch, like, and share the below video we have created to help educate prescribers at EASIL facilities on the new LRI guidelines. EASIL staff created this with the help of Dr. Sujit Suchindran, an infectious diseases physician and healthcare epidemiologist at Emory University.
LRI Guidelines
EASIL has developed clinical algorithms that are based on the most recent literature on LRI treatment in LTCFs. This source material presents the underlying evidence-base for changes in clinical practice that are shown to reduce patient harm for those suffering from LRI.
Community Acquired Pneumonia (CAP)
Nursing Home Acquired Pneumonia (NHAP)
Other LRI Guidelines
2016 University of Rochester Pneumonia Guidelines
University of Nebraska general duration of therapy for various conditions
2) Utilize best antibiograms to inform prescribing
Local Susceptibility
When considering antibiotics for treatment of LRI in LTCFs, antibiograms can help you optimize your drug regimen for regional variation in pathogen susceptibility. EASIL has partnered with the Clinical Laboratory Services, Inc. (CLS) to provide up-to-date antibiograms for the Southeastern region.
3) Pre-prescription actions
SBAR
Situation, Background, Assessment, Recommendation
SBARs are completed by nurses to help communicate with prescribing physicians about the status of patients and indication or contraindication for antibiotics.
SBARs in Stewardship
To learn more about how to use a SBAR in stewardship, download this How-to Guide from Nebraska Medicine.
Division of Healthcare Quality Promotion CDC Resources
for Healthcare Professionals
4 ) Post-prescription actions
List of potential actions from CDC's Core Elements on Stewardship
Re-evaluate the utility of antibiotics with more information
Often antibiotics are started in patients with suspected UTI or LRI based on exclusively empirical information. After lab result are delivered, clinicians should re-evaluate the utility of antibiotics and their indication with respect to prescription criteria. Often, de-escalation or discontinuation is indicated after re-evaluation.
Antibiotic stewardship programs should have triggers in place to prompt re-evaluation when appropriate. For more information, visit Appendix A of CDC's Core Elements document linked above.
Loeb's criteria checklist courtesy of Nebraska Department of Public Health
Chart reviews help to evaluate how well prescribers adhere to best practices for antibiotic starts
When performing a facility review, it is important to evaluate every case systematically using the same tool to avoid introducing bias. EASIL suggests using the Loeb's criteria checklist linked above.